Scalp Psoriasis Explained: Symptoms, Causes, and Relief Options
Scalp psoriasis is a chronic skin condition that can cause itching, flaking, and discomfort. In this article, we explore the key symptoms, possible causes, and treatment options that can help manage flare-ups and improve your quality of life without making exaggerated claims.
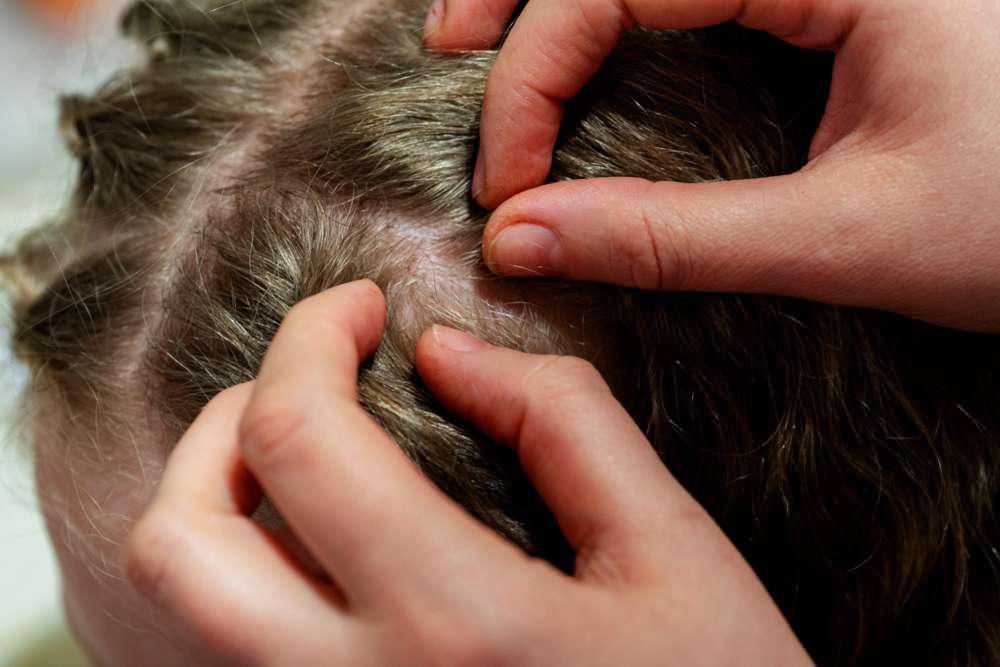
Scalp psoriasis is a form of plaque psoriasis that primarily affects the scalp, hairline, behind the ears, and the back of the neck. It is not contagious. Instead, the immune system speeds up skin cell turnover, creating thick, inflamed plaques that shed scales. While it can resemble stubborn dandruff, scalp psoriasis usually forms well-defined plaques with silvery-white scales and can cause soreness, tightness, or burning. Effective relief typically combines medicated treatments with careful daily care and trigger awareness.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What are the common symptoms of scalp psoriasis?
Scalp psoriasis often starts with well-demarcated patches of redness covered by dry, silvery scales. Itching can range from mild to intense and may disrupt sleep. Some people experience a burning or stinging sensation, and removing scales too aggressively can lead to pinpoint bleeding. Hair shedding can occur during flares, typically from scratching and inflammation, but the condition itself does not scar hair follicles. Plaques may extend beyond the scalp onto the forehead, neck, or around and inside the ears. Compared to dandruff, which tends to be greasy and diffuse, scalp psoriasis is thicker, drier, and more sharply bordered.
What triggers scalp psoriasis flare-ups?
Common triggers include psychological stress, cold or dry weather, and skin injury (known as the Koebner phenomenon), such as scratching, tight hairstyles, or harsh hair treatments. Infections—particularly streptococcal throat infections—may worsen psoriasis in some individuals. Certain medications can be associated with flares, including lithium, some beta-blockers, and antimalarials; discuss any concerns with a healthcare professional before changing a prescription. Alcohol misuse and smoking are also linked to more frequent or severe flare-ups. Fragrant or harsh shampoos, heavy gels, and vigorous brushing can irritate plaques and prolong symptoms.
Most effective treatment options for scalp psoriasis
First-line care often includes topical therapies. High-potency corticosteroids (for example, in solutions, foams, gels, or medicated shampoos) reduce inflammation quickly. Vitamin D analogs (calcipotriol/calcipotriene) and steroid–vitamin D combinations can enhance control while allowing lower steroid exposure. Keratolytics such as salicylic acid help lift thick scales so medications can penetrate. Coal tar preparations are sometimes used for anti-inflammatory and anti-itch benefits. For extensive or unresponsive disease, targeted phototherapy (narrowband UVB combs) or systemic treatments may be considered. Systemic options include oral agents (such as methotrexate, cyclosporine, acitretin, or apremilast) and biologics that target specific immune pathways. Treatment choice depends on severity, affected areas, medical history, and personal preference.
How to manage scalp psoriasis flare-ups at home
A gentle routine can improve comfort and support medical therapy. Before shampooing, soften scales with mineral oil or a salicylic acid preparation for 10–20 minutes; then massage gently to lift flakes without picking. Use medicated shampoos exactly as directed—often allowing a few minutes of contact time before rinsing—and alternate with a mild, fragrance-free shampoo to reduce irritation. Keep nails short to minimize damage if you scratch. Avoid tight hats or hairstyles that rub plaques, and use soft-bristled brushes. Track triggers in a simple journal, noting stress, product changes, climate shifts, or illness. Brief, sensible sun exposure may help some people, but protect unaffected skin and avoid burns. Many find that stress-reduction strategies—such as regular exercise, mindfulness, or counseling—reduce flare frequency and intensity.
Which treatments do dermatologists prescribe?
Dermatologists commonly prescribe high-potency topical corticosteroids for short, targeted courses—such as clobetasol propionate 0.05% in foam, solution, lotion, or shampoo—or betamethasone dipropionate in similar vehicles. Calcipotriol/calcipotriene solutions and fixed-dose steroid–vitamin D combinations are frequent maintenance choices. For thick plaques, keratolytics (for example, salicylic acid) can be added to improve medication penetration. Intralesional corticosteroid injections may be used for stubborn localized plaques. When scalp involvement is severe, widespread, or significantly affects quality of life, systemic therapies may be recommended, including methotrexate, cyclosporine, acitretin, apremilast, or biologics that target TNF, IL‑17, or IL‑23 pathways. Phototherapy with a UVB comb can be an alternative when appropriate. Decisions are individualized based on disease extent, response to prior treatments, other health conditions, and preferences, ideally discussed with a dermatologist in your area.
Relief from scalp psoriasis typically comes from combining the right medical treatments with steady, gentle self-care. Recognizing symptoms early, understanding personal triggers, and adjusting routines can reduce flare intensity and duration. Over time, many people find a sustainable plan that keeps plaques controlled, itch manageable, and the scalp comfortable, even as the condition naturally waxes and wanes.